Prostate Cancer Treatment Options
If you have been diagnosed with a prostate cancer you will have discussed the treatment options in detail with your Urologist. In general there are 3 widely acceptable common forms of treatment.
Curative treatment can be achieved by either surgery (radical prostatectomy) or by radiation. In recent years a 3rd form of treatment known as active surveillance has become much more accepted. Active surveillance is possible for cancers that are considered to be of low volume and low grade i.e. non aggressive, and in these circumstances it is believed that immediate treatment is not required. This form of treatment will require regular checks of your PSA, as well as repeat prostate biopsies at specified intervals. If the PSA begins to rise or repeat biopsies demonstrate an increase in the volume or grade of cancer then definitive therapy would be indicated. You will need to discuss your particular cancer details in detail with your Urologist to determine whether or not you are suitable for active surveillance.
ROBOTIC PROSTATECTOMY
Robotic prostatectomy refers to removal of the prostate by key hole surgery. The surgeon sits at a console next to the patient and controls robotic arms attached to instruments inside the patient’s abdomen. This allows extremely fine movements of the instruments and the magnified 3-D view can make the surgery easier and more precise. Patients generally have a shorter stay in hospital with less post operative pain. The general risks and complications however, are similar to those of open surgery.
The major risks and potential complications associated with radical prostatectomy are listed in the consent menu.
RADICAL PROSTATECTOMY
Radical prostatectomy involves removal of the entire prostate gland that sits between the bladder and the urethra (water pipe). No matter how this procedure is performed (open surgery or laparoscopic / keyhole / robotic technique) the procedure is essentially the same. The major factors to be considered with this treatment are the rare risk of severe incontinence, the risk of erectile dysfunction and the possibility that further treatment may be required if microscopic disease is left behind after the surgery
In most cases patients regain a high degree urinary control. There are well described pelvic floor exercises that will be explained to you prior to the surgery and these will help your continence improve following the procedure. After the operation you will have a catheter to drain urine from the bladder while the join between the bladder and the urethra heals. An X-ray (cystogram) will be performed within a week and if the join has sealed the catheter can be removed.
The nerves that initiate and maintain erections are located in very close proximity to the side of the prostate. In many circumstances these nerves can be peeled off the prostate (nerve sparring procedure). Theoretically this would preserve your erectile function.
You will need to have a very careful discussion with your Urologist about your suitability for a nerve sparring procedure. Patients must be aware that even with a nerve sparring procedure erectile function is not guaranteed and patients expectations should be realistic in this regard. Factors contributing to post operative erectile dysfunction include age, whether one or two nerves can be spared and other technical factors identified at the time of surgery. Medications can be used to aid in erectile function following the surgery for penile rehabilitation if required.
Following surgery the prostate tissue is sent to the pathology department for microscopic examination. If tumour is found to be present at the margin or edge of the prostate or specimen then it would be assumed that microscopic tumour still remains in the patient i.e. a positive margin. In certain circumstances no immediate treatment is required and the PSA will be monitored. In some low grade tumours further treatment may never be required. In more aggressive tumours, however, further treatment in the form of radiation may be required to mop up any residual tumour and this will need to be discussed in detail with your Urologist and with a Radiotherapist.
Click here to read more about consent issues related to Radical prostatectomy.
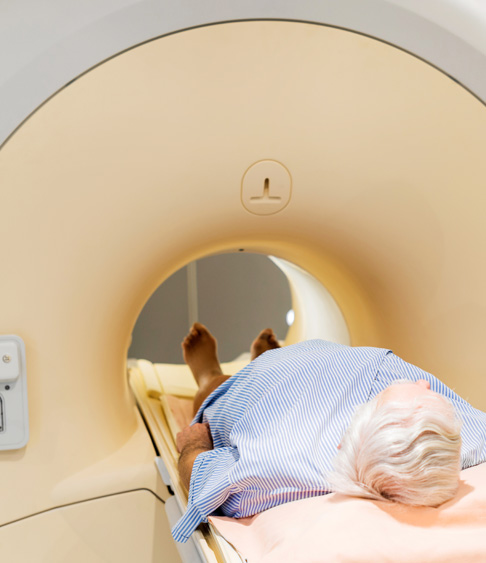
RADIATION THERAPY
For many men with prostate cancer, radiotherapy is an effective treatment alternative. Radiotherapy has a different profile of side effect including erectile dysfunction and bladder and bowel irritation from radiation but in general is tolerated extremely well.
Some patients are not suited for radiation therapy. Very young men with prostate cancer generally should not be offered radiation due to the risk of the cancer recurring while they are still relatively young. In this situation, surgery following radiation is extremely difficult and has a higher risk of severe incontinence and bleeding due to the tissue damage associated with radiation. Other tumour factors may also make radiation less likely to cure disease.
Radiation can be delivered in several ways including external beam therapy, seed brachytherapy or high dose brachytherapy. The pros and cons of each of these should be discussed with you prior to deciding on a particular treatment method.
Most men can be treated with curative intent with both surgery and radiation. As a patient, each man needs to weigh up the potential side effects of each treatment modality and decide which method of treatment he is most comfortable with. You Urologist can guide you in making the choice but you should feel comfortable with the treatment option you chose, and not feel pressured one way or another if several options are available.
