Prostate MRI and New Biopsy Techniques
Prostate MRI is becoming more and more important in the diagnosis and management of prostate cancer. It is important, however, to interpret an MRI correctly and use the information in conjunction with other data such as your PSA and other risk factors for prostate cancer. MRI can be used in the initial diagnosis of cancer but is also used when following men with cancer who do not require treatment immediately after diagnosis ie – in active surveillance. In these men, changes in the MRI appearance of the prostate over time may indicate change or progression in their cancer which may result in a repeat biopsy or even a decision to treat the cancer sooner rather than continue with observation.
Understanding the MRI Scan
It is important to understand what the MRI scan can detect. It will not show all cancers and in fact generally only shows more aggressive, high grade tumours. This means it will not detect low grade, slow growing cancers. This is generally a good thing as it is these non- aggressive cancers that may well not require treatment soon, or in fact ever. They can generally be observed over time and treated if there is suspicion of progression.
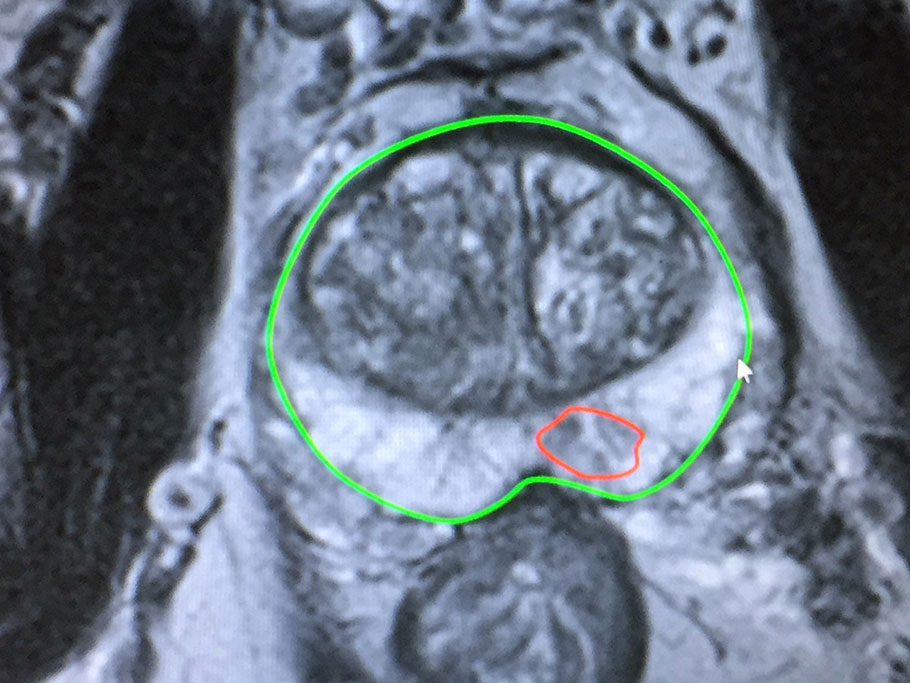
If a suspicious lesion is identified on an MRI scan, it will be graded according to the likelihood that it represents a significant cancer. This is called the PIRADS score. A PIRADS score of 4 or 5 indicates a high suspicion of significant disease that will likely require treatment. A lesion with a score of PIRADS 3 has about a 50:50 chance of significant disease.
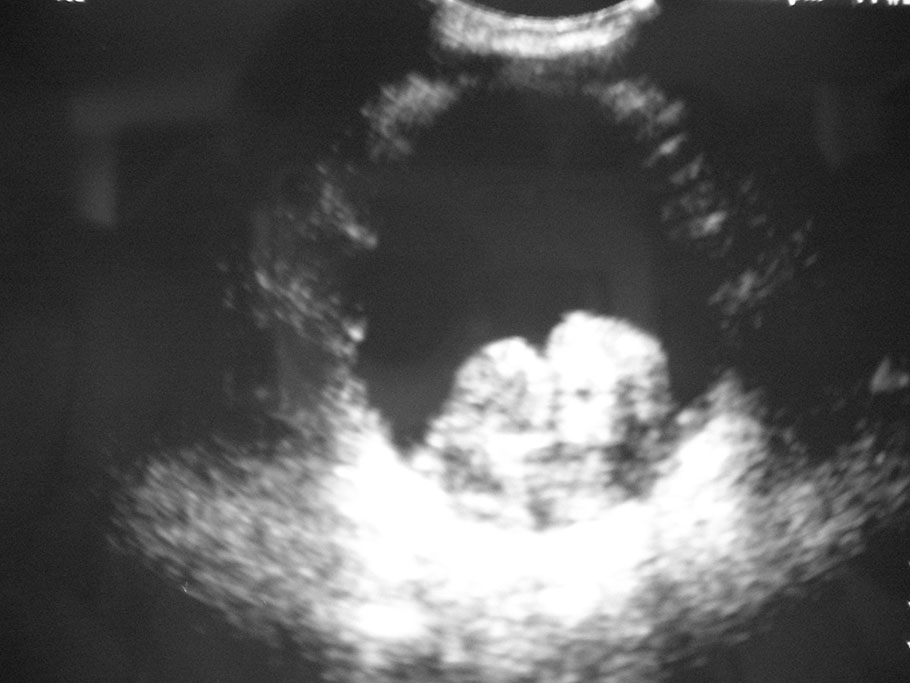
If a suspicious lesion is identified, it can be targeted specifically at the time of biopsy by a technique called MRI fusion biopsy. This technique fuses the MRI image with the ultrasound image used when performing biopsy to allow us to more accurately biopsy the abnormal area.
MRI also gives the Urologist information about whether or not a cancer has extended beyond the capsule of the prostate which helps to plan the surgery more carefully. This can have implications if nerve sparing surgery in being contemplated. It may also detect enlarged lymph nodes near the prostate that may indicate spread of disease.